THE VASCULAR ENDOTHELIAL GROWTH FACTOR-A GENE POLYMORPHISM PREDICTS CLINICAL OUTCOMES AMONG ACUTE ST-SEGMENT ELEVATION MYOCARDIAL INFARCTION PATIENT
Inna M. Kutia 1, Mykola P. Kopytsya 2, Yaroslava V. Hilova 1, Olga V Petyunina 3, Alexander E. Berezin 4*
|
|
|
ABSTRACT
Context: Vascular endothelial growth factor (VEGF) is an angiopoetic factor, the variability of circulating level of which is mediated by expression of specific VEGF-A gene variants. Aims: To investigate the predictive role of VEGF-A gene polymorphism for clinical outcomes in ST-segment elevation myocardial infarction (STEMI) patients. Settings and Design: An open prospective single-center cohort study. Methods and Material: 135 patients with acute STEMI and 30 healthy volunteers were enrolled in the study. The G634C polymorphism in the VEGF-A gene was performed by real-time polymerase chain reaction at baseline. The 6-month combined clinical endpoint was determined. Statistical analysis used: The univariate and multiple variate log-regression analysis. Results: The entire patient population was distributed into two groups depending on G634G-genotype (n = 70) and combination with G634C and C634C-genotypes (n=65). Unadjusted multivariate regressive logistic analysis has shown peak troponin I at admission, Killip class of heart failure > 2, GC/CC polymorphisms in VEGF-A gene, dynamic increased NT-proBNP and VEGF-A levels for 6 months, and remained independent predictors for the combined endpoint. After adjustment for dynamic changes of NT-proBNP and VEGF-A levels, the GC/CC polymorphisms in the VEGF-A gene remained an independent predictor of clinical outcome. Kaplan-Meier curves have demonstrated that GG VEGF-A genotype was associated with a lower frequency of combined endpoint when compared with GC/CC VEGF-A genotypes (Log-rank p = 0.02). Conclusions: The G634C polymorphism in the VEGF-A gene was found as an independent predictor for 6-month combined endpoints amid STEMI patients.
Keywords: ST-segment elevation myocardial infarction, single nucleotide polymorphism G634C, vascular endothelial growth factor, prediction, outcomes
Introduction
Patients with acute ST-segment myocardial infarction (STEMI) undergoing successful primary percutaneous coronary intervention (PCI) yield significant difference with in-hospital mortality, hospital length of stay, cardiovascular (CV) events and complications, and late survival [1, 2]. Previous systematic network meta-analysis has shown that multivessel coronary artery disease (CAD) in STEMI patients is a much more powerful trigger than single-vessel CAD for survival and prognosis regardless of revascularization strategy [3]. Additionally, complete revascularization based on a comprehensive condition is disputed as the best-fitted choice in the actual clinical situation including hemodynamic instability, newly onset heart failure, and high risk of severe short-term CV complications [4, 5]. However, a staged revascularization strategy is recommended for complex non-infarct-related artery lesions under evaluation (fractional flow reserve, intravascular ultrasound, optical coherent tomography) [6, 7]. The long-term risk of CV events and severity of left ventricular post-MI remodeling remain to be uncertainly predictable after successful PCI with TIMI-III restoring of blood flow through the culprit artery and even after complete revascularization [8, 9]. As a result, STEMI patient complexity undergone primary successful PCI has not changed significantly.
Numerous studies have revealed that effective angiogenesis and neovascularization play a crucial role in the early restoration of microvascular perfusion in damaged myocardium and prevention of late left ventricular remodeling for months after re-perfused STEMI [10-12]. Vascular endothelial growth factor A (VEGF-A) is a key regulator of angiogenesis [13-15], which mediates pro-angiopoetic, anti-inflammatory, and anti-oxidative capacities acting via appropriate receptors [16, 17]. VEGF is generated by thyroid follicles due to long term stimulation of thyroid-stimulating hormone (TSH) receptor (TSHR). VEGF activates its receptors on endothelial cells in thyroid, causing thyroid gland hypervascularization [18, 19]. The VEGF-A synthesis and secretion are mediated by hypoxia through over-expressed hypoxia-induced factor-1 and nuclear factor-kB [17]. VEGF-A contributes to the development of collaterals by increasing vascular permeability, stimulating proliferation and migration of progenitor and mature endothelial cells, inhibition of apoptosis of endothelial precursors, production of matrix metalloproteinases, and activation of von Willebrand factor [20].
Previous studies have shown that the levels of VEGF-A in patients with acute STEMI were significantly higher than in healthy volunteers [21]. After PCI, the concentration of biomarkers showed a dramatic decrease by approximately 70% with the most profound decline seen in individuals with the highest initial VEGF-A concentrations [22]. There is strong evidence regarding the negative predictive value of lowered circulating levels of VEGF-A and major cardiovascular events (MACEs) after STEMI for a one-year observation [23]. Interestingly, circulating levels of VEGF-A exhibited severe variability in healthy volunteers as well as in patients with STEMI and this result was determined by functional G634C (rs 2010963) polymorphism in VEGF-A gene [24, 25]. We hypothesized that functional variant of rs 2010963 VEGF-A gene can determine dynamic changes of VEGF-A levels after PCI and potentiate endogenous repair system activity to protect damaged myocardium after STEMI from microvascular obstruction improving long-term prognosis. The aim of the study was to investigate the predictive role of rs 2010963 VEGF-A gene polymorphism for clinical outcomes in STEMI patients after complete successful PCI.
Subjects and Methods:
Patients’ population
A total of 190 patients with confirmed acute STEMI were analyzed for participation in the study (Figure 1). From the entire population of STEMI (n=190) according to inclusion and non-inclusion criteria, we enrolled 140 individuals with acute STEMI who were admitted to the intensive care unit of “L.T.Malaya TNI NAMSU” (Kharkiv, Ukraine) within a given period from 2016 January to 2019 June. Acute STEMI was diagnosed according to ECS Guidelines (2017) [26]. Thirty healthy volunteers were enrolled as a control group.
Figure 1: Study design flow chart
Inclusion criteria were established acute STEMI, age > 18 years old, a lack of contraindications to PCI, and written informed consent to participate in the study. Exclusion criteria were previous myocardial infarction, established chronic heart failure, severe comorbidities (anemia, chronic obstructive lung disease, bronchial asthma, liver cirrhosis, chronic kidney disease with declined glomerular filtration rate < 35 mL/min×1.73m2, valvular heart disease, and bleeding), known malignancy and pregnancy, and inability to understand the informed consent.
Primary PCI with bare-metal stent (COMMANDER, “Alvimedica”, Turkey) implantation was performed in 104 patients within 6-12 hours after initial acute STEMI confirmation in V.T. Zaytsev Institute of General and Emergency Surgery NAMSU (Kharkiv, Ukraine). Systemic thrombolysis (tPA tenecteplase i.v. bolus per conventional protocol) was carried out in 31 STEMI patients before PCI. All acute STEMI patients received adjuvant treatment due to current ESC recommendations [26]. TIMI III blood flow restoring through the culprit artery was determined for every re-perfused patient with acute STEMI (Figure 2).
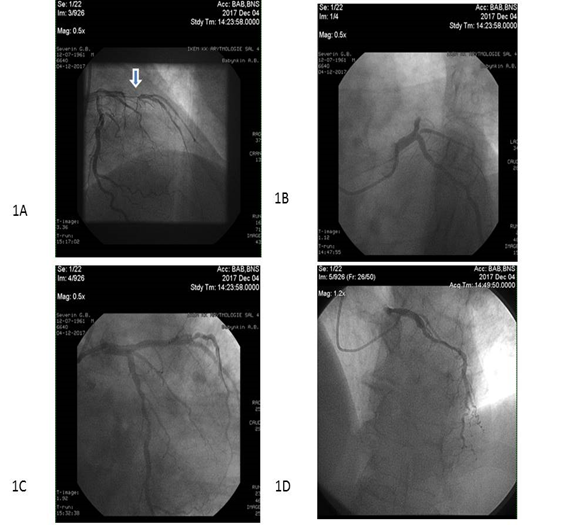
Figure 2: Complete revascularization in STEMI patients. Occlusion (arrow) and TIMI III blood flow restoring through culprit artery with PCI (1A and 1B, respectively) and reperfusion through ischemia-relating stenosis (1C and 1D)
Ethical declaration
All procedures performed in the study involving human participants were in accordance with the ethical standards and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards and approved by the local ethics committee (Protocol №6, 30.05.2017). Written voluntary informed consent was obtained from each patient before entering the study.
Sample size calculation
The sample size was calculated through the effect size estimation (0.99), the type of present study, providing study power of 80% and type I error 5%, STEMI in-hospital mortality of 7.5%, and one-year mortality of 14% [27]. The sample size was 135 individuals.
Coronary angiography
Conventional coronary angiography was performed immediately after admission of the patients to the hospital using Digital X-Ray system “Integris Allura” (Philips Healthcare, Best, The Netherlands) and managed by radial or femoral vascular access. Coronary arteries were visualized with two-to-three orthogonal projections per conventional protocol. The number of views obtained was decided by the operator depending on coronary anatomy. The main coronary arteries were left main coronary artery, left anterior descending branch, left circumflex branch, right main coronary artery, and right coronary descending branch. In this study, the contrast “Ultravist-370” (Baier Pharma GmbH, Germany) and automatic contrast injector were used. The contrast amount used in coronary angiography in each injection was 8-10 mL at 4 mL/s for the left coronary artery and 6 mL at 3 mL/s for the right coronary artery (radiation exposure 20 to 35 mGycm). After coronary angiography, two experienced interventional cardiologists discussed the captures and filled in the final report of the results of the procedure after reaching consensus.
Determination of risk factors and comorbidities
Hypercholesterolemia (HCE) was diagnosed if total cholesterol (TC) level was above 5.2 mmol/L, and/or low-density lipoprotein cholesterol (LDL) level was above 3.0 mmol/L, and/or level of triglycerides (ТG) was above 1.7 mmol/L according to with European Cardiology Society dyslipidemia guideline (2016) [28]. Hypertension was diagnosed if systolic blood pressure (SBP) was >140 mm Hg, and/or diastolic blood pressure (DBP) >90 mm Hg according to European guidelines on diagnostics and treatment of arterial hypertension (2018) [29]. Heart failure was diagnosed according to ESC guidelines for the diagnosis and treatment of acute and chronic heart failure (2016) [30]. Positive smoking history was defined as having smoked daily or occasionally in the past.
Transthoracic Echocardiography and Doppler
Transthoracic echocardiography was performed on “Aplio 500” (TUS-A500) TOSHIBA MEDICAL SYSTEMS CORPORATION with the usage of 3.5 MHz phase probe at discharge and at 6-month observation period. Left ventricular (LV) end-diastolic volume (LVEDV), LV end-systolic volume (LV ESV), and LV ejection fraction (LVEF) measuring were done according to Simpson's method per contemporary recommendation. Left atrial diameter (LAD) and left atrial volume (LAV) was determined according to the contemporary protocol [31]. LV myocardial mass (LVMM) was calculated in an automatic manner per protocol of echocardiograms evaluation. LV global longitudinal strain (e`) and early transmitral velocity (E) were measured by tissue Doppler imaging technique and impulse transmitral Doppler regime at baseline and at 6 months per protocol.
Determination of STEMI prognosis
We used the TIMI score to validate prognostic capacity after STEMI [32].
SYNTAX score determination
SYNTAX score (SS) was used to assess the severity of coronary atherosclerotic lesions, and it was calculated by experienced interventional cardiologist accordingly [33].
Determination of endpoint
The endpoint was determined as the combined event included CV death, recurrent angina, and newly diagnosed heart failure for 6 months after PCI. CV death was ascertained by personal or phone contact with the family doctor or the hospital where the patient died. The diagnosis of recurrent angina required the presence of clinical signs/symptoms or electrocardiographic changes. Hospitalization was ascertained by direct contact or phone call to the hospital reception where the patient was admitted. The discharge report or autopsy report was obligatory reviewed before endpoint determination.
Blood samples
Blood samples were drawn immediately before PCI and at 6 months after acute STEMI. Blood samples were centrifuged; serum was isolated within 30 min of sample acquisition and freezed at -70°C and stored in plastic tubes until being shipped to the laboratory of immune-chemical and molecular-genetic researches of “L.T.Malaya TNI NAMSU” (Kharkiv, Ukraine).
N-terminal brain natriuretic peptide (NT-proBNP) levels were measured with a commercial kit for ELISA manufactured by Vector-Best (Russia Federation).The NT-proBNP level average was 0.05-2000 pg/mL.
The levels of troponin I (Tn I) and creatin kinase-isoenzyme-MB (CK-MB) were measured with chemo luminescent immunoassay on Humalyser 2000 (Mannheim, Germany). The TnI and CK-MB levels averages were 0.5-50 ng/mL and 0-500 mmol/L. The intra-assay and inter-assay coefficients of variation were <5%.
The levels of VEGF-A were measured with a commercial kit for ELISA produced by (IBL International GMBH, Germany). The VEGF-A level average was 0 to 1000 pg/mL. The intra-assay and inter-assay coefficients of variation were <5%.
High-sensitive C-reactive protein (hs-CRP) levels in serum were measured with a commercially available standard kit (R&D Systems GmbH, Wiesbaden-Nordenstadt, Germany). The hs-CRP level average was 0-100 mg/L.
Total cholesterol (TC), low-density lipoprotein (LDL) cholesterol, high-density lipoprotein (HDL) cholesterol, and triglycerides (TG) were measured with a direct enzymatic method (Roche P800 analyzer, Basel, Switzerland). The intra-assay and inter-assay coefficients of variation were <5%.
SNP G634G (rs 2010963) in VEGF-A gene determination
The DNA extraction was performed from peripheral blood leukocytes according to the protocol for a commercial system «CFX96 Touch» (BioRad Laboratories Pte.Ltd., Сінгапур) using appropriate RT-PCR kit produced by Syntol (Russia Federation). Genotyping of the G634C VEGF-A gene polymorphism located in the promoter region was performed using primers and probes using real-time (RT) polymerase chain reaction (PCR). Primers that we used in VEGF-A (rs 2010963) polymorphism assay were GAGAGAAGT CGAGGAAGAGAGAGA-3′ (forward primer), CCCAAAAGCAGGTCA CTCACTT-3′ (reverse primer), VEGF-A-FAM-5′- CCTGTCCCTTTCGC-3′, and VEGF-A-VIC-5′- CCTGTCGCTTTCGC-3′.
Statistics
Statistical analyses were performed using SPSS for Windows v.23 (USA). Continuous variables are presented as mean ± standard deviation (SD) when normally distributed, or median and interquartile range (IQR) if otherwise. Categorical variables are presented as frequencies (n) and percentages (%). Mann-Whitney and Wald-Wolfowitz's criteria were used for intergroup differences and quantitative values. The qualitative variables are expressed as percentages and were compared with the χ2 test and the exact F Fisher test. Allele frequencies were estimated, and all polymorphisms were tested for Hardy–Weinberg Equilibrium. Correlations between G634G VEGF-A gene polymorphism, angiographic characteristics, hemodynamic performances, and biomarkers were received using rang correlation r Spearmen test. We performed univariate and multiple variate log-regression analysis to determine variables that predict endpoint and cardiac remodeling. Beta coefficient, standard errors (SE), odds ratio (OR), 95% confidence interval (CI) for each factor were estimated. Factor, for which P values were calculated as >0.5 were not included in the multiple variate log-regression analysis. Survival analysis for clinical outcomes was performed using Kaplan–Meier curves and the log-rank test. All differences were considered statistically significant with 2-tailed P<0.05.
Results:
The observed frequencies of variants of G634C VEGF-A (rs 2010963) genotype among entire STEMI patient population (n=135) were GG=51.9% (n=70), GС = 47.4% (n=64), and CC=0.7% (n=1) respectively. There was a deviation from Hardy–Weinberg equilibrium due to an excess of heterozygosity (χ2=10.9, P=0.00099). Healthy volunteers (n=30) had GG VEGF-A (rs 2010963) genotype in 53% (n=16); CT VEGF-A (rs 2010963) genotype in 43% (n=13); and CC VEGF-A (rs 2010963) genotype in 4% (n=1) without significant deviation from expecting frequencies (χ2=0.726, P=0.394). The circulating levels of VEGF-A in healthy volunteers and STEMI patients at baseline depending on G634C VEGF-A (rs 2010963) genotypes are reported in Figure 3.
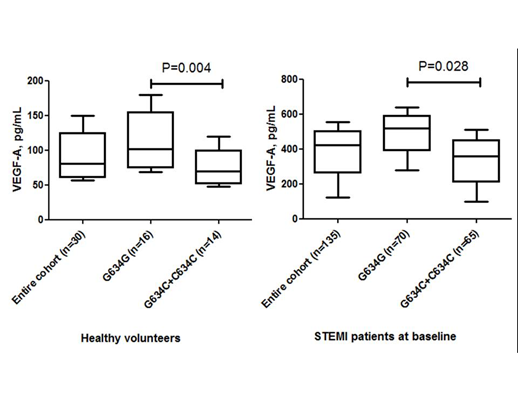
Figure 3: The circulating levels of VEGF-A in healthy volunteers and STEMI patients depending on G634C VEGF-A (rs 2010963) genotypes.
There were no significant differences between both STEMI patient cohorts in age, sex, CV risk factors (hypertension, dyslipidemia, abdominal obesity, type 2 diabetes mellitus, smoking, and premature CV events in family anamnesis) (Table 1). Therefore, we did not find sufficient differences between frequencies in atrial fibrillation, stable and unstable angina prior to STEMI, as well as II-IV Killip classes of heart failure, GRACE and TIMI scores’ points in both patient cohorts. Additionally, baseline medications were similar in both STEMI patient cohorts. However, STEMI patients with GG variant of the VEGF-A gene rarely presented anterior localization of myocardial infarction (MI) and frequently presented posterior localization of MI of individuals with GC/CC VEGF-A genotypes, while there was no difference in right main coronary artery injury between cohorts (Table 2). On the contrary, STEMI patients with GC/CC VEGF-A genotypes had frequently left main coronary artery injury.
Table 1: Baseline characteristics of the patient included in the study.
|
Variables |
Entire population (n=135) |
Patients with GG genotype (n=70) |
Patients with GC and СС genotypes (n=65) |
c2, Р value |
|
Age, years |
59.2± 8.92 |
59.30±8.50 |
59.69±8.85 |
c2 =0.03; p=0.639 |
|
Sex, male/female, n (%) |
109/26 (80.7 / 19.3) |
57/13 (81.4 / 19.6) |
52/13 (80.0 /20.0 ) |
c2 =0.04; p=0,833 |
|
Hypertension, n (%) |
110 (81.5) |
56 (80.0) |
54 (83.1) |
c2 =0.21; p=0.646 |
|
Dyslipidemia, n (%) |
35 (25.9) |
19 (27.1) |
18 (27.7) |
c2 =0.22; p=0.688 |
|
Abdominal obesity, n (%) |
28 (20.7) |
13 (18.5) |
15 (23.0) |
c2 =0.82; p=0.218 |
|
Type 2 diabetes mellitus, n (%) |
33 (24.4) |
15 (21.4) |
18 (27.7) |
c2 =0.72; p=0.398 |
|
Smoking, n (%) |
65 (48.1) |
33 (47.1) |
32 (49.2) |
c2 =0.06; p=0.808 |
|
Premature CV events in family anamnesis, n (%) |
72 (53.3) |
38 (54.3) |
36 (55.4) |
c2 =0.02; p=0.898 |
|
Stable angina prior to STEMI, n (%) |
49 (36.3) |
20 (28.6) |
29 (44.6) |
c2 =3.75; p=0.053 |
|
Unstable angina prior to STEMI, n (%) |
46 (34.1) |
19 (27.1) |
27 (41.5) |
c2 =3.11; p=0.078 |
|
Atrial fibrillation, n (%) |
10 (7.4) |
4 (5.7) |
6 (9.4) |
c2 =0.59; p=0.326 |
|
II-III Killip classes of HF, n (%), |
26 (19.3) |
12 (17.1) |
14 (21.5) |
c2 =0.42; p=0.518 |
|
IV Killipclass of HF, n (%) |
11 (8.1) |
7 (10.0) |
4 (6.2) |
c2 =0,67; p=0.414 |
|
Risk scores |
||||
|
GRACE Score, points |
150 (120-172) |
143 (117-170) |
152 (119-176) |
P=0.294 |
|
TIMI score, points |
6 (4-7) |
6 (4-7) |
7 (5-8) |
P=0.66 |
|
Baseline medications |
||||
|
Beta-blocker, n (%) |
125 (92.6) |
66 (94.3) |
59 (90.8) |
c2 =0.22; p=0.762 |
|
ACEI, n (%) |
61 (45.1) |
29 (41.4) |
32 (49.2) |
c2 =2.25; p=0.068 |
|
Ticagrelor, n (%) |
135 (100) |
70 (100) |
65 (100) |
c2 =0.016; p=0.92 |
|
Statins, n (%) |
135 (100) |
70 (100) |
65 (100) |
c2 =0.016; p=0.92 |
Notes: Data are reported as n (%), mean ± standard deviation, and median (interquartile range). Mann-Whitney and Wald-Wolfowitz's criteria were used for intergroup differences and quantitative values, respectively.
Abbreviations: ACEI, angiotensin-II converting enzyme inhibitor; HF, heart failure.
Table 2: STEMI localization and angiographic characteristics.
|
Variables |
Entire population (n=135) |
Patients with GG genotype (n=70) |
Patients with GC and СС genotypes (n=65) |
c2, Р value |
|
STEMI localization |
||||
|
Anterior wall, n (%) |
59 (43.7) |
24 (34.3) |
35 (53.8) |
c2 =5.24 p=0.022 |
|
Posterior wall, n (%) |
53 (39.3) |
34 (48.6) |
19 (29.2) |
c2 =5.29 p=0.022 |
|
Other, n (%) |
23 (17.0) |
12 (17.1) |
11 (16.9) |
c2 =0.001 p=0.973 |
|
Infarct-related coronary artery |
||||
|
Left main coronary artery, n (%) |
7 (5.2) |
1 (1.4) |
6 (9.2) |
c2 =4.17 p=0.041 |
|
Right main coronary artery, n (%) |
27 (20.0) |
10 (14,3) |
17 (26,2) |
c2 =2.97 p=0.085 |
|
Circumflex coronary artery, n (%) |
17 (12.6) |
9 (12.9) |
8 (12.3) |
c2 =0.01 p=0,923 |
|
Anterior interventricular artery, n (%) |
31 (23.0) |
12 (17.1) |
19 (29.2) |
c2 =2.78 p=0.095 |
Notes: Data are reported as numbers and percentages.
Table 3 reported baseline cardio dynamic characteristics and biomarkers in the patients of the study population. STEMI patients with GC/CC VEGF-A genotypes had significantly increased LVEDV, LVESV, and E/e` ratio at baseline in comparison with patients who had GG VEGF-A genotype. We did not determine differences between patients’ cohorts in GFR, serum creatinine, peak TnI, CK-MB, NT-proBNP, lipid profile, and hs-CRP, but circulating levels of VEGF-A were profoundly lower in STEMI patients who had GC/CC VEGF-A genotypes.
Table 3: Baseline cardio dynamic characteristics and biomarkers in patients of the study population.
|
Variables |
Entire population (n=135) |
Patients with GG genotype (n=70) |
Patients with GC and СС genotypes (n=65) |
Р value |
|
Hemodynamics |
||||
|
SBP, mm Hg |
135±22 |
135±24 |
136±27 |
0.428 |
|
DBP, mm Hg |
80±12 |
79±13 |
82±14 |
0.154 |
|
LVEDV, mL |
147±25 |
138±31 |
151±33 |
0.044 |
|
LVESV, mL |
68±24 |
63±23 |
73±31 |
0.039 |
|
LVEF, % |
50±10 |
51±13 |
49±10 |
0.250 |
|
E/e`, units |
12.50±1.17 |
10.20±1.21 |
13.90±1.60 |
0.046 |
|
LVMMI, g/m2 |
149.30±44.32 |
148.78±46.82 |
157.28±47.10 |
0.607 |
|
Biomarkers |
||||
|
Creatinine, μmol/L |
98.13 [86.90-119.30] |
96.75 [86.30-113.20] |
104.40[88.10-123.60] |
0.274 |
|
GFR, ml/min |
69.67 [58.40-87.63] |
71.00 [61.00-89.00] |
67.50[56.00-88.00] |
0.445 |
|
hs-CRP, mg/L |
12.04±4.77 |
11.82±5.19 |
12.53±5.03 |
0.531 |
|
VEGF-A, pg/mL |
420.81 [123.76–553.19] |
314.01 [159.94-627.66] |
221.28 [77.58-440.82] |
0.045 |
|
Peak TnI, ng/ml |
18.4 [5.44-77.3] |
17.70 [6.77-99.00] |
23.07 [4.07-75.50] |
0.914 |
|
CK-MB, mmol/L |
106.80 [51.20-290.40] |
121.05 [42.30-275.05] |
87.00 [44.90-300.10] |
0.458 |
|
NT-proBNP, pmol/L |
480.26 [116.81–1558.31] |
219.34 [75.70-440.82] |
515.56 [109.91-1727.77] |
0.821 |
|
Lipid profile |
||||
|
TC, mmol/l |
4.95 [3.97-5.71] |
4.97 [3.98-5.64] |
4.91 [4.10-5.63] |
0.85 |
|
HDL, mmol/l |
1.09 [0.90-1.28] |
1.12 [0.90-1.31] |
1.14 [0.90-1.20] |
0.761 |
|
LDL, mmol/l |
3.00 [2.11-3.71] |
2.97 [2.11-3.67] |
3.01 [2.07-3.99] |
0.303 |
|
TG, mmol/l |
1.53 [1.17-2.02] |
1,90 [1.19-2.06] |
1.61 [1.13-1.91] |
0.023 |
Notes: Data are reported as n (%), mean ± standard deviation, and median [interquartile range]. Mann-Whitney and Wald-Wolfowitz's criteria were used for intergroup differences.
Abbreviations: SBP, systolic blood pressure; DBP – diastolic blood pressure; LVEDV – left ventricular end-diastolic volume; LVESV - left ventricular end-systolic volume; LVEF – left ventricular ejection fraction; LVMM – left ventricular myocardial mass; LDL, low-density lipoprotein; HDL, high-density lipoprotein; TG – triglycerides; Tn, cardiac troponin; hs-CRP, high sensitive C-reactive protein; GRF, glomerular filtration rate; VEGF-A, vascular endothelial growth factor; NT-proBNP, N-terminal brain natriuretic peptide; CK-MB, creatine kinase isoform MB.
Six-month observation revealed that cardiac hemodynamic performances and levels of cardiac biomarkers (hs-CRP, VEGF-A, NT-proBNP) were similar in both patients’ cohort, while E/e` ratio was significantly increased in patients with GC/CC VEGF-A genotypes (Table 4). Dynamic changes of VEGF-A and NT-proBNP levels in STEMI patients with variants of G634C VEGF-A polymorphism for 6 months are reported in Figure 4. Patients with GC/CC VEGF-A genotypes have been demonstrated both lowered 6-month levels of VEGF-A and increased 6-month levels of NT-proBNP of individuals with GG VEGF-A genotype. Therefore, we found that within 6 month period, 29 cases of pre-specified clinical outcomes have occurred (9 cases and 20 cases in GG VEGF-A genotype and GC/CC VEGF-A genotypes cohorts, respectively). Interestingly, a significant difference between cohorts was received in frequencies of MI, but not in other reasons for clinical outcomes.
Table 4: 6-month cardio dynamic characteristics, levels of biomarkers, and clinical outcomes in patients of study population.
|
Variables |
Entire population (n=135) |
Patients with GG genotype (n=70) |
Patients with GC and СС genotypes (n=65) |
Р value |
|
Hemodynamics |
||||
|
SBP, mm Hg |
132±15 |
136±22 |
130±14 |
0.186 |
|
DBP, mm Hg |
82±12 |
82±14 |
82±11 |
0.484 |
|
LVEDV, mL |
155±20 |
145±39 |
158±31 |
0.261 |
|
LVESV, mL |
78±24 |
70±25 |
81±39 |
0.308 |
|
LVEF, % |
50±8 |
52±8 |
49±12 |
0.220 |
|
E/e`, units |
13.30±1.17 |
10.90±1.18 |
15.70±1.25 |
0.038 |
|
Biomarkers |
||||
|
hs-CRP, mg/L |
9.82±4.00 |
8.54±3.20 |
10.43±4.10 |
0.662 |
|
VEGF-A, pg/mL |
406.70 [210.50-523.71] |
424.56 [230.60-556.93] |
330.24 [162.80-472.14] |
0.129 |
|
NT-proBNP, pg/mL |
388.29 [151.70-920.50] |
280.29 [81.39-718.34] |
540.01 [461.99-1217.31] |
0.074 |
|
Clinical outcomes |
||||
|
Admission due to HF, n (%) |
6 (4.4) |
1 (1.4) |
5 (7.7) |
0.088 |
|
MI, n (%) |
14 (10.4) |
5 (7.1) |
9 (13.8) |
0.048 |
|
Death, n (%) |
9 (6.7) |
3 (4.3) |
6 (9.2) |
0.160 |
|
Total, n (%) |
29 (21.4) |
9 (12.9) |
20 (30.8) |
0.020 |
Notes: Data are reported as n (%), mean ± standard deviation, and median [interquartile range]. Mann-Whitney and Wald-Wolfowitz criteria were used for comparisons
Abbreviations: SBP, systolic blood pressure; DBP – diastolic blood pressure; LVEDV – left ventricular end-diastolic volume; LVESV - left ventricular end-systolic volume; LVEF – left ventricular ejection fraction; hs-CRP, high sensitive C-reactive protein; GRF, glomerular filtration rate; VEGF-A, vascular endothelial growth factor; NT-proBNP, N-terminal brain natriuretic peptide; HF, heart failure.
Correlations between G634G VEGF-A gene polymorphism, angiographic characteristics, hemodynamic performances, and biomarkers
There were positive correlations between GC/СС VEGF-A genotype and combined endpoint (r=0.58; P=0.0001), dynamic increased NT-proBNP level for 6 month (r=0.42; P=0.001), SYNTAX score (r=0.34; P=0.001), anterior STEMI (r=0.36; P=0.003), LDL cholesterol (r=0.22; P=0.032), TIMI score (r=0.26; P=0.012), atrial fibrillation (r=0.28; P=0.001), unstable angina prior to STEMI (r=0.25; P=0.047), E/e` ratio (r=0.23; P=0.048) and multiple coronary vessels injury (r=0.26; P=0.002), and inverted correlation with dynamic increased VEGF-A level for 6 month (r=-0.42; P=0.001), and LV ejection fraction (r=-0.33; P=0.001) in acute STEMI patients.
Therefore, we found a correlation between LV ejection fraction and dynamic increased NT-proBNP (r=-0.48; P=0.003) and VEGF-A level for 6 months (r=0.46; P=0.003) in STEMI patients with GC/CC VEGF-A genotypes, but it was not confirmed in patients with GG variant of VEGF-A genotype. Yet, multiple coronary artery injury correlated to LV ejection fraction at baseline (r=0.33; P=0.001), NT-proBNP (r=0.32; P=0.001), dyslipidemia (r=0.30; P=0.002), type 2 diabetes mellitus (r=0.28; P=0.001), hs-CRP (r=0.26; P=0.001), E/e` ratio at baseline (r=0.24; P=0.002), abdominal obesity (r=0.23; P=0.024), smoking (r=0.22; P=0.046), and male sex (r=0.22; P=0.048). There were no significant associations between the GG variant of VEGF-A genotype and the prevalence of traditional CV risk factors.
Determination of predictors for 6-month clinical endpoint
The univariate linear regression (stepwise) analysis has allowed verifying peak TnI at admission, TIMI score, abdominal obesity, Killip HF class > II at admission, anterior localization of STEMI, atrial fibrillation, GC/CC variants of VREGF-A gene, NT-proBNP at baseline, and dynamic changes for levels of NT-proBNP and VEGF-A in serial measures as predictors for the combined clinical endpoint (Table 5). Other variables did not embed into multivariate regressive analysis due to P>0.1.
Unadjusted multivariate regressive logistic analysis has shown peak TnI at admission, Killip class of HF > 2, GC/CC polymorphisms in VEGF-A gene, dynamic increased NT-proBNP and VEGF-A levels for 6 months and remained independent predictors for the combined endpoint (Table 5). After adjustment for dynamic changes of NT-proBNP and VEGF-A levels for 6 months, we found that GC/CC polymorphism in the VEGF-A gene was an independent predictor of poor clinical outcomes (β-coefficient=1.6635; odds ration =2.8244; 95% confidence interval = 1.2649 – 11.2972; P=0.0001).
Table 5: The factors contributing 6-month combined endpoint after STEMI: The results of univariate and multivariate linear regressions.
|
Variable |
Depending variable: combined clinical endpoint |
|||||||
|
Univariate linear regressive analysis (c2 =61.293; Р< 0.0001) |
Multivariate linear regressive analysis (c2 =32.140; Р < 0.0001) |
|||||||
|
β-coefficient |
OR |
95% CІ |
Р |
β-coefficient |
OR |
95% CІ |
Р |
|
|
Peak TnІ at admission |
-1.8578 |
1.0111 |
1.0007 – 1.0215 |
0.0358 |
-0.012610 |
1.0127 |
1.0016 – 1.0239 |
0.0247 |
|
Peak CK-MB at admission |
0.47640 |
1.0254 |
1.0180 – 1.104 |
0.4820 |
- |
|||
|
SYNTAX score |
0.98677 |
1.0028 |
1.0002 – 1.006 |
0.6884 |
- |
|||
|
TIMI score |
1.37250 |
1.8970 |
0.9720 – 2.880 |
0.0410 |
1.17280 |
1.0940 |
1.010 – 1.3240 |
0.0520 |
|
Killip class of HF >II |
0.9874 |
1.3725 |
0.0536 – 2.5869 |
0.3179 |
2.23331 |
9.3307 |
2.4408 – 35.6689 |
0.0011 |
|
Smoking |
-0.49898 |
0.6071 |
0.0328 – 11.2510 |
0.7376 |
- |
|||
|
Dyslipidemia |
0.4582 |
0.8848 |
0.6638 – 1.1255 |
0.6388 |
- |
|||
|
T2DM |
2.98372 |
19.7611 |
0.8341 – 46.1875 |
0.0647 |
- |
|||
|
Abdominal obesity |
1.12320 |
2.1448 |
0.4607 – 3.8995 |
0.0383 |
1.02 |
1.9560 |
0.0774 – 3.4539 |
0.0526 |
|
Stable angina prior to STEMI |
0.43968 |
1.5522 |
0.3988 – 6.0419 |
0.5260 |
- |
|||
|
Unstable angina prior to STEMI |
1.55459 |
0.2113 |
0.0149 – 2.9884 |
0.2501 |
- |
|||
|
Anterior STEMI |
1.98807 |
7.3014 |
1.1181 – 47.6782 |
0.0378 |
1.85810 |
5.2064 |
0.0122 – 21.4412 |
0.0586 |
|
Atrial fibrillation |
1.00347 |
0.1349 |
0.0157 – 1.1565 |
0.0476 |
1.00254 |
0.1104 |
0.0120 – 1.1433 |
0.0662 |
|
Multiple coronary vessel injury |
1.37022 |
3.9362 |
0.8228 – 18.8312 |
0.0862 |
- |
|||
|
GC/CC polymorphisms in VEGF-A gene |
5.89420 |
2.9263 |
1.5366 – 5.3407 |
0.0199 |
1.72401 |
5.6070 |
1.4777 – 21.2745 |
0.0113 |
|
E/e` at baseline |
0.35360 |
0.9160 |
1.0136 – 1.1630 |
0.0870 |
- |
|||
|
NT-proBNP at baseline |
1.18440 |
1.7044 |
1.0633 – 2.954 |
0.03420 |
1.17230 |
1.0144 |
1.0330 – 1.1422 |
0.0620 |
|
Dynamic increased NT-proBNP level for 6 month |
1.21370 |
1.8692 |
1.1354 – 4.8264 |
0.02427 |
1.09377 |
1.2177 |
1.0464 – 3.5569 |
0.0357 |
|
Dynamic increased VEGF-A level for 6 month |
-0.005467 |
1.0055 |
1.0007 – 1.0103 |
0.0241 |
-0.0015896 |
1.0016 |
1.0002 – 1.0029 |
0.0201 |
Abbreviations: OR, odds ratio; T2DM, type 2 diabetes mellitus; CAD, coronary artery disease; LDL, low-density lipoprotein; LV, left ventricular; VEGF-A, vascular endothelial growth factor; NT-proBNP, N-terminal brain natriuretic peptide; E - early transmitral velocity; e` - global longitudinal LV strain.
Kaplan-Meier analysis for endpoint accumulation trends in STEMI patients with variants of VEGF-A genes
Kaplan-Meier curves have demonstrated that STEMI patients with GG VEGF-A genotype had a lower frequency of clinical combined endpoint accumulation when compared to those who had GC/CC VEGF-A genotypes (Log-rank p = 0.02) (Figure 4).
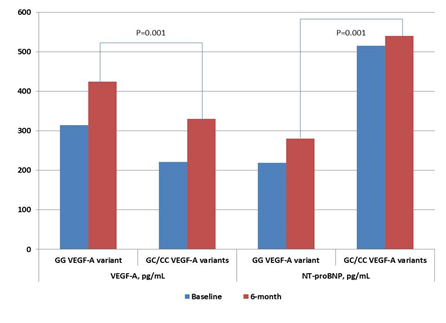
Figure 4: Dynamic changes of VEGF-A and NT-proBNP levels in STEMI patients with variants of G634C VEGF-A polymorphism for 6 months.
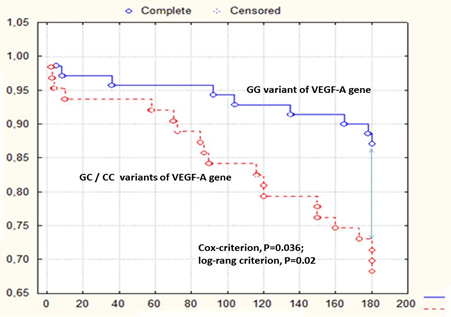
Figure 5: Kaplan-Meier curve accumulation of combined endpoint after 6-month observation depending on polymorphism G634C in the VEGF-A gene.
Discussion:
The results of our study maintain the hypothesis that the GG variant of the VEGF-A gene is able to mediate myocardial protection via higher levels of VEGF-A in peripheral blood prior to STEMI as well as for 6 months after this event. Consequently, GC/CC variants of the VEGF-A gene, which were associated with lowered basic and post-event levels of VEGF-A, have demonstrated close relation to the accumulation of combined clinical endpoints for 6 months. We first revealed that complete revascularization in STEMI patients having GC/CC variants of the VEGF-A gene can draw unexpectedly worse clinical results for a follow-up than that appears in patients with GG variants of VEGF-A gene. Interestingly, at baseline both STEMI patients’ cohorts did not significantly differ from each other in traditional CV risk factors, several biomarker levels (including CRP and NT-proBNP), the severity of coronary atherosclerosis, while left main coronary artery injury was determined frequently in patients with GC/CC variants of VEGF-A gene. Previous animal and clinical studies have shown that VEGF-A exhibited powerful cardiac reparative effects, protected from ischemia/reperfusion injury, reduced myocardial edema and MI size; also, cardiac macrophages recruited by pro-inflammatory cytokines were certain conductors of these protective impacts [34-36]. Moreover, VEGF-A levels were independently associated with microvascular obstruction during STEMI [36]. However, our results may indirectly confirm evidence regarding that the VEGF-A acting as protector of endovascular edema and microvascular obstruction prevented adverse LV remodeling. Indeed, Ferraro B et al (2019) reported that the VEGF-A levels were significantly and inversely correlated with LVEF at 6-month follow-up. Our results are well corresponded to this evidence, while we did not find a strong correlation between the VEGF-A levels at baseline and LVEF at baseline. However, there were strong interrelations between GG VEGF-A genotype and circulating levels of VEGF-A. Probably, the role of variants of the VEGF-A gene has been become crucial for the post-event period and corresponded to maintaining a higher VEGF-A level in peripheral blood to prevent adverse LV remodeling through a lowered risk of distal coronary obstruction [37]. However, angiographic parameters and coronary anatomy in STEMI patients who were effectively treated with primary PCI with TIMI-III restoring blood flow and re-perfused completely did not strongly correlate to a risk of late microvascular obstruction, which remained an independent predictor of LV remodeling, mortality following STEMI, and all-cause mortality even after further adjustment for infarct size [38, 39]. In this context, a prediction of follow-up survival during STEMI treated effectively with PCI seems to be a credible tool for risk stratification of STEMI patients and GC/CC VEGF-A genotypes could be discussed as a prognosticator for poor clinical outcomes. However, there is no optimal methodology that best predicts the surrogate outcome marker of LV function and survival in post-STEMI patients [39, 40].
The strength of our investigation is the enrollment of the STEMI patients with normal and preserved LVEF that were candidates for complete re-perfusion therapy with PCI. There are limiting data, which were able to predict CV events and late LV remodeling in post-STEMI individuals without a clinically significant decline in LV pump function and symptomatic HF [41]. The results of our study have revealed that the presentation of GC/CC variants of the VEGF-A gene predicted a good tendency to worsening LFEF and worsening LF diastolic filling. These results may be interpreted in a context of late microvascular obstruction that frequently follows complete PCI. Indeed, our results showed that a combined clinical endpoint was occurred predominantly due to new MI, but not other reasons. Probably, GC/CC variants of the VEGF-A gene were not able to support vascular protection with adequate VEGF-A production after STEMI and protected microvascular obstruction, which led to MI in the follow-up period [42]. It has been unleashed that STEMI patients who are suggested microvascular obstruction had higher peak TnT and lower LVEF because of an increased LVEDV [43]. Despite an association between GC/CC variants of VEGF-A gene, and risk of CAD and quality of life in the general population was determined previously [44, 45], there were not close associations between severity of atherosclerosis, the number of damaged coronary artery and GC/CC VEGF-A genotype in STEMI patient population [46]. On the contrary, there are other findings, which are clarified positive associations between the culprit artery lesion localization, MI size, and microvascular obstruction [47, 48]. Because there are close interrelationships between VEGF-A tissue expression and serum levels, microvessel density, ROS production, and expression of vascular endothelial cadherin in re-perfused myocardium [49], the role of variants of VEGF-A genotypes in tissue protection in STEMI are markedly suggested. In this context, the exact molecular mechanisms, which mediate the causative relation of VEGF-A to vascular and myocardium protection in post-STEMI patients are not clearly understood. It has been postulated that elevated levels of VEGF-A in post-STEMI patients is a result of myocardial ischemia/hypoxia, induced by microvascular dysfunction after distal coronary artery embolization and vascular inflammation. In fact, early microvascular obstruction is accompanied by declining of LVEF, whereas late microvascular dysfunction in post-STEMI individuals can be associated with LV diastolic dysfunction without reduced LVEF [50, 51]. Large clinical studies are required to clearly understand the role of genetic polymorphism of the VEGF-A gene in mediating endogenous reparation and tissue protection. However, we believe that the determination of GC/CC VEGF-A genotype could provide relevant prognostic insights leading to improved short-term and long-term risk stratification in STEMI patients treated with complete revascularization.
There are several study limitations. First, a small sample size does not allow providing analysis in detail in subgroups and additionally interpreting causes that led to appear MACEs directly related to new MI. Secondary, it would be optimal to use late gadolinium-enhanced magnetic resonance images to determine an interrelationship between microvascular obstruction and an increased risk of adverse CV events in post-STEMI patients. Third, it has remained not fully understood whether attenuated plaque and well-positioned stent were causes for adverse outcomes. Yet, we have measured total VEGF-A levels, but we did not determine the fractions of VEGF-A, which were found to be provided different impacts on myocardium and vasculature. Finally, we believe that these study limitations will not be able to diminish sufficiently the value of the results of our investigation.
Conclusion:
The G634C polymorphism in the VEGF-A gene was found as an independent predictor for 6-month clinical combined endpoints in STEMI patients after primary successful PCI.
References
