EXPERIENCE OF CARRYING OUT MAGNETIC RESONANCE IMAGING WITH THE USE OF SPECIALIZED PROTOCOLS AND PROGRAMS COMPUTER POST-PROCESSING
Ya. S. Shevchenko1, D. P. Plohova1, I.N. Bulakhova2, A. E. Mishvelov3*, M.E. Kubalova4, G. B. Badriev4, Kh. A. Mildzikhov4, A. N. Simonov5, M. N. Verevkina5, A.I. Okolelova6, S.N. Povetkin7
|
|
- 526B group of Pediatric Faculty, Stavropol State Medical University, Russian Federation.
- Department of radiology, Stavropol Regional Clinical Consulting and Diagnostic Center, Russian Federation.
- Laboratory of 3D technologies, Stavropol State Medical University, Russian Federation
- Medical Faculty, North Ossetian State Medical Academy, Russian Federation.
- Department of Epizootiology and Microbiology, Stavropol State Agrarian University, Russian Federation.
- Department of Anatomy, Veterinary Obstetrics and Surgery, Kuban State Agrarian University, Russian Federation.
- Institute of Life Systems, North Caucasus Federal University, Russian Federation.
|
ABSTRACT
The article considers a clinical case with various kidney neoplasms using magnetic resonance imaging, which were processed by different methods in the HoloDoctor and Slicer.DoctorCT software package. There are also examples of diagnostics of relapse when performing magnetic resonance imaging in a patient with kidney resection for renal cell cancer in their own clinical practice.
Keywords: HoloDoctor, Slicer.DoctorCT, Renal cell carcinoma, Magnetic resonance imaging, Dynamic contrast enhancement, Relapse
Introduction
Tumors are of the main causes of deaths worldwide [1-3]. When planning an operation, the location of tumors concerning surgically significant vessels and neighboring organs is of paramount importance [4-13]. An equally important factor is the ability to estimate the volume of the tumor in relation to the tissue. Previously, three-dimensional visualization is reported for interactive planning of operations for complex liver resections, while there are isolated cases when planning operations on the pancreas, but there is no data on the use of this method for kidney operations [14-16]. Andrén et al. (2006) have shown that three-dimensional reconstruction of the pancreas with semi-automatic segmentation can be created similarly to liver imaging.
To solve these problems, the HoloDoctor software package was created. The software package consists of three main modules: an Anatomical Atlas module, a Data analysis module, and a Surgical planning simulation module [16-19]. The Anatomical Atlas module allows you to solve the problem of high-quality training of new medical personnel (students of medical universities). The module is an interactive Anatomical Atlas of organs, which includes three-dimensional models of structures of organs, organs and systems of human organs in normal and pathological conditions. The Data analysis module allows you to view DICOM images of various studies (CT, MRI, MSCT, etc.). Like the Anatomical Atlas module, it can be used for teaching students (as viewing information on the example of clinical cases), and for practicing physicians.
The article considers a clinical case with various kidney neoplasms using magnetic resonance imaging, which were processed by different methods in the HoloDoctor and Slicer.DoctorCT software package. There are also examples of diagnostics of relapse when performing magnetic resonance imaging in a patient with kidney resection for renal cell cancer in their clinical practice.
Material and Methods
Computer tomography for non-specific back pain in a patient (59 years old) revealed a volume formation of the left kidney. The disease was asymptomatic, although at the time of detection it had a significant size. Surgical intervention was performed in the volume of resection (June 2018). Histological examination of the preparation of a remote segment of the kidney determined light-cell renal cell carcinoma G4.
Further, the dynamic observation was performed using radiation diagnostic methods (ultrasound, computed tomography, magnetic resonance imaging) with a frequency of 1 every 3 months. The patient did not complain during the observation period. At the level of surgical intervention, the fibrosis zone was determined, which was natural. The next scheduled MRI–scan (November 2019) revealed changes that were different from those that occurred earlier.
Preparation for the MRI: specific preparation was not required. The patient was explained the need to perform commands to hold her breath and remain motionless while being in the magnet tunnel. A peripheral catheter was inserted into the left cubital vein, and a breath sensor was connected.
MRI was performed on a PHILIPS Ingenia 1.5 Tesla high-field MRI scanner using a standard special protocol [8] that includes:
- T2, T2 cor, synchronized with the respiratory cycle, cut thickness 3.0 mm (0.3).
- T2-SPIR Ah, synchronized with the respiratory cycle, cut thickness 3.0 mm (0.3).
- T1 on phase/out phase Ah, synchronized with the respiratory cycle, cut thickness 3.0 mm (0.31).
- Div Ah with b-factors 0, 100, 800, 1200 with ADC map construction, slice thickness 3.0 mm (0.3).
- T1-fs TRIVE Ah, thin-section (3D), synchronized with the respiratory cycle, with bolus contrast injection (Multihens 0.5% 0.2 ml per kg of weight, at a rate of 4.0 ml/s), in dynamic contrast enhancement mode: native series, late arterial phase (at 15s), venous phase (at 50s), parenchymal (at 3min), with subsequent construction of perfusion graphs, color mapping.
- T1-fs DRIVE car, thin-cut (3D), synchronized with the respiratory cycle.
Computer post-processing of MRI scans was obtained by the HoloDoctor and Slicer.DoctorCT software package [20-23].
Results and Discussion
MRI showed the following results:
- No clearly defined additional formations were found in the structure of the postoperative scar against the background of fibrotic changes in the anatomical structures (Fig. 1).
- The study revealed a rounded zone of 11,0×10,0 mm in functional sequences with the following characteristics of the MRI signal:
- The glow area on the DVI is at high factors, the IR signal is heterogeneous, and the diffusion restriction is moderate (Fig. 2).
- Early accumulation of contrast in the arterial phase (Fig. 3)
- The pathological zone has quite clear contours, and there is no capsule.
- Solid structure, without necrosis and hemorrhage, on T2, T2-SPIR and T1 characteristics do not differ from scar tissue.
- In the analysis of images in addition to visual assessment (increased MRI signal in the area of interest in the arterial phase) used a program of postprocessing (T1 perfusion), which allows performing the mapping (Fig. 4) and plot the accumulation of the contrast (Fig. 5). For comparison with the area of interest (Roi 1) the selected portion of cortical substance (Roi 2) and renal artery (Roi 3). The graphs made it possible to clearly see the difference in blood supply. In the area of interest, the rate of contrast accumulation was slightly lower than in the arteries but higher than in the cortical substance. In addition, rapid contrast removal was demonstrated (type 1 curve). Thus, the pathological zone was considered as hypervascular relative to the renal parenchyma.
- Localization of the pathological zone near the kidney gate could indicate the involvement of the calico-pelvic system, but the small volume of changes and location in the scar left this fact at the level of assumption.
- There were no changes in the contralateral kidney and other parts of the ipsilateral kidney.
- Lymph Nodes in the area of the kidney gate, retroperitoneal lymph nodes were not enlarged.
- The Cup-pelvis-plating system of the ipsilateral kidney was not dilated.
- There was no infiltration of paranephral fiber.
- Signs of secondary liver lesions were not available.
Taking into account the appearance of a solid pathological site with signs of hypervascularity and limited diffusion in it (which is an indicator of high cellularity) in the zone of postoperative scar changes, which was not previously detected during dynamic observation, a conclusion was made about recurrent tumor growth. The patient underwent a nephrectomy. Histological examination of the removed kidney in the area of the lower pole near the sinus revealed a rounded formation of 10.0 mm in diameter – a light-cell renal cell carcinoma G2-G3 with growth into the wall of the pelvis. There are foci of fibrosis in the adjacent parenchyma. Thus, the changes detected during the MRI completely coincided with the histological conclusion.
Figure 1 – Area of fibrous postoperative changes, relatively homogeneous tissue.
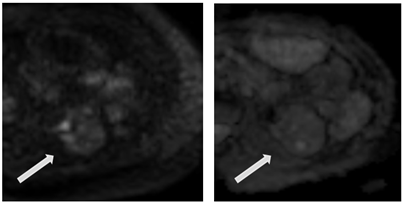
Figure 2 – The glow Area on the DWI (diffusion-weighted images). The MDK (measured diffusion coefficient) signal is heterogeneous, and the diffusion restriction is moderate.
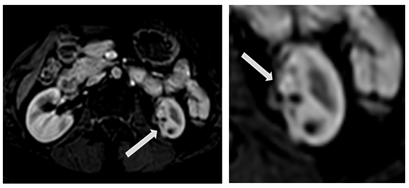
Figure 3 – Visual previously accumulated contrast in the area of interest (arterial phase).
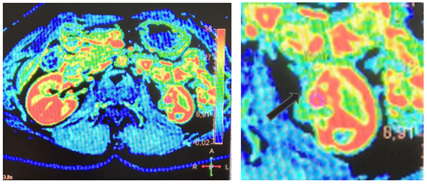
Figure 4 – Color mapping, the color in the area of interest differs from other areas that have accumulated contrast (blood vessels, kidney cortex).
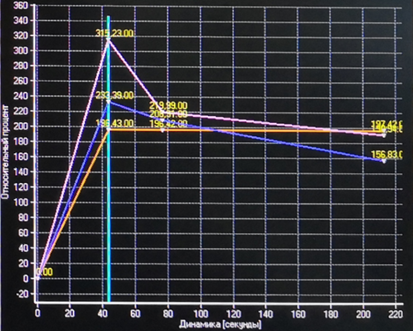
Figure 5 – Contrast accumulation Graphs:
the upper one is in the renal artery,
average – in the pathological zone,
lower – in the cortical substance.
Conclusion
Magnetic resonance imaging in a patient with kidney resection for renal cell carcinoma using specialized protocols and computer post-processing programs revealed a recurrence of cancer, which had a small size and was located against the background of the postoperative scar. In this situation, dynamic contrast enhancement performed at optimal time intervals was crucial in differential diagnostics. Previously, the accumulation of contrast (hypervascularity) in the area of relapse reflected pathological blood flow, the process of neoangiogenesis.
The study of the postoperative material of the resected kidney fully confirmed the conclusions made based on the MRI. At the moment, the developed software package is used by doctors in the Department of Radiology and Short-term Surgical Hospital of the Stavropol Regional Clinical Consulting and Diagnostic Center according to the developed technological cycle and has successfully proved itself among doctors of various fields.
References
- Al-Bishri W M. Alleviating Impact of Α-Lipoic Acid And Silver Nanoparticles on 1,2- Dimethylhydrazine Dihydrochloride Induced Hepatic Carcinogenesis. Int. J. Pharm. Phytopharm. Res. 2017; 7(6): 44-5
- Kirsha K S, Karuvallil S M, Rachel R. Case Report on Operative Management of Pheochromocytoma. Int. J. Pharm. Phytopharm. Res. 2019; 9(3): 44-47.
- Negahi A, Boozari B, Vaziri M, Mousavie S H, Farazmand B. Pancreatic head tumor revealing as a Schwannoma: A case report. J. Adv. Pharm. Edu. Res. 2019; 9(S2): 101-105.
- Andrén O, Fall K, Franzén L, Andersson S O, Johansson J E, Rubin M A. How well does the Gleason score predict prostate cancer death? A 20yearfollowup of a population based cohort in Sweden. J Urol. 2006;175: 1337–1340. doi: 10.1016/S00225347(05)007342
- Areshidze DA, Mischenko DV, Makartseva LA, Kucher SA, Kozlova MA, Timchenko LD, Rzhepakovsky IV, Nagdalian AA, Pushkin SV. Some Functional Measures of the Organism of Rats at Modeling of Ischemic Heart Disease in Two Different Ways. Entomology and Applied Science Letters. 2018 Jan 1;5(4):19-29.
- Association of Oncologists of Russia. Clinical recommendations for the diagnosis and treatment of kidney cancer/Moscow, 2014.
- Russian Society of Urology Russian Society of Oncourology. Association of Oncologists of Russia Russian Society of Clinical Oncology. Clinical recommendations. Kidney parenchyma cancer/ Moscow, 2018.
- Ljungberg B, Albiges L, Abu-Ghanem Y, Bensalah K, Dabestani S, Fernández-Pello S, Giles RH, Hofmann F, Hora M, Kuczyk MA, Kuusk T. European Association of Urology Guidelines on Renal Cell Carcinoma: The 2019 Update. (2019). EURURO-8276– 12 p.
- Medical Mistakes Kill 100,000+ Americans A Year. Journal of the American Medical Association. Electronical source: http://www.yourmedicaldetective.com/drgrisanti/dangerous_medicine.htm
- Nagdalian A.A., Selimov M.A., Topchii M.V., Oboturova N.P., Gatina Yu.S., Demchenkov E.L. Ways to reduce the oxidative activity of raw meat after a treatment by pulsed discliarge technology. Research Journal of Pharmaceutical, Biological and Chemical Sciences. 2016. 7(3): 1927-1932.
- Pushkin SV, Nagdalian AA, Rzhepakovsky IV, Povetkin SN. AFM and CT Study of Zophoba Smorio Morphology and Microstructure, Entomol Appl Sci Lett, 2018, 5 (3): 35-40.
- Iyer RK, Chiu LL, Vunjak-Novakovic G, Radisic M. Biofabrication enables efficient interrogation and optimization of sequential culture of endothelial cells, fibroblasts and cardiomyocytes for formation of vascular cords in cardiac tissue engineering. Biofabrication. 2012 Jul 31;4(3):035002.
- Sayf Al-Katib, MD, Monisha Shetty, MD, Syed Mohammad A. Jafri, MD, Syed Zafar H. Jafri, MD. Radiologic Assessment of Native Renal Vasculature: A Multimodality Review, RG • 37(1): 136-156.
- Mishvelov EG, Melchenko EA, Vlasov AA, Anfinogenova OI, Nuzhnaya CV. Holodoctor Planning Software Real-Time Surgical Intervention, Pharmacophore, 2019; 10(2), 1-12.
- Osipchuk GV, Povetkin SN, Ashotovich A, Nagdalian IA, Rodin MI, Vladimirovna I, Ziruk AN, Svetlakova EV, Basova NJ, Rzhepakovsky IV, Areshidze DA. The Issue of Therapy Postpartum Endometritis in Sows Using Environmentally Friendly Remedies”, Pharmacophore, 2019; 10(2): 82-84.
- Hight GY, Mishvelov AE, Melchenko EA, Nuzhnaya CV, Epanov VA, Dolgalev AA, Kukharuk MY, Portnov MY, Suprunchuk VE. New Image Modeling Features For Planning Surgical Interventions. Research Journal of Pharmaceutical, Biological and Chemical Sciences. 2019, 10 (1):140-143.
- Bledzhyants GA, Mishvelov AE, Nuzhnaya KV, Anfinogenova OI, Isakova JA, Melkonyan RS, Hite GY, Suprunchuk VE, Makova AV, Popov AN, Ovechkin VS. The Effectiveness of the Medical Decision-Making Support System "Electronic Clinical Pharmacologist" in the Management of Patients Therapeutic Profile”, Pharmacophore, 2019; 10(2), 76-81.
- Nuzhnaya KV, Mishvelov AE, Osadchiy SS, Tsoma MV, AM RS, Kurbanova KA, Rodin IA, Nagdalian AA, Rzhepakovskiy IV, Piskov SI, Povetkin SN. Computer Simulation and Navigation in Surgical Operations, Pharmacophore, 2019; 10(4): 43-48
- Sizonenko MN, Timchenko LD, Rzhepakovskiy IV, DA SP, Areshidze VV, Nagdalian AA, Simonov AN, Svetlakova EV, Verevkina MN, Povetkin SN. The New Efficiency of the «Srmp» – Listerias Growth-Promoting Factor during Factory Cultivation”, Pharmacophore, 2019; 10(2), 85-88.
- Selimov MA, Nagdalian AA, Povetkin SN, Statsenko EN, Litvinov MS, Mishvelov AE. Investigation of CdCl2 Influence on red blood cell morphology, Int. j. pharm. phytopharm. Res. 2019; 9(5): 8-13
- I. O. Sokolova, O. V. Ivanov, D. A. Belyakov, T. B. Belyakova Creation and use of the program for studying the anatomy of the human cardiovascular system with the function of augmented reality, Scientific forum: Innovative science: collection of articles on materials VIII international conference. Moscow 2017, 7(8): 26-30.
- Stalling, D.; Westerhoff, M.; Hege, H.-C. C.D. Hansen and C.R. Johnson, ed. "Amira: A Highly Interactive System for Visual Data Analysis". The Visualization Handbook. Elsevier: 2005: 749–767. doi:10.1016/b978-012387582-2/50040-x
- Sovilj, S., Magjarevic, R., Lovell, N., Dokos, S. Realistic 3D bidomain model of whole heart electrical activity and ECG generation // Computing in Cardiology. 2013; 40: 377–380.




