THE MARGINAL ADAPTATION OF DIFFERENT ZIRCONIA REINFORCED CERAMIC SYSTEMS: A SYSTEMATIC REVIEW
Rakan Yousef Alrashdan1*, Ahmed Sultan Alharbi1, Anas Mohamed Baghareeb1, Hamad Suliman Alatiah1, Khaled Saeed Alqahtani1, Zaki Fakiha2
|
|
|
ABSTRACT
Purpose: This study aimed to review the published literature examining the accuracy of the marginal fit of the zirconia crown and comparing the marginal adaptation between various systems to identify which of them would achieve better marginal conformity. Materials and Methods: A literature review for articles published in the PubMed and Scopus databases was undertaken in February 2020, utilizing explicitly determining inclusion and exclusion criteria. A total of 560 publications were identified, and 330 omitted after screening the title and abstract. After a full-text study, another 214 publications were removed, allowing 16 articles to be used in the final review. The fit refers to the mean marginal gaps in the sample, and the precision is the fit minus the pre-set spacer. Result: The overall mean fit values of Zirconia systems were 67μm, and the accuracy was calculated to be 36μm, which is in the clinically desirable range. Conclusion: All the Zirconia systems considered in this study produced marginal discrepancy in the clinically desirable range.
Keywords: Marginal accuracy, Marginal fit, Marginal gap, Marginal discrepancy, Fitting accuracy, Zirconia crown
Introduction
In recent decades, increasing demand from patients for natural-appearing dental restorations has led to the evolution of all ceramic materials with enhanced mechanical characteristics that have better durability. These are currently substituting traditional metal-ceramic restorations. Further, CAD/CAM technology development makes it possible for making such materials. [1–3] Since introducing the CAD/CAM technology in the 1980s computer system has been extensively utilized to design, develop, and shape materials into various forms [4-7]. Mormann was credited for introducing commercially designed CAD/CAM (Cerec, Sirona Dental Systems).[8]
Zirconia is considered as one of the materials milled by CAD/CAM. Zirconia is a kind of ceramics that can occur in many forms without a glassy phase. It is in a monoclinic crystalline form at room temperature, which is changed into a tetragonal and cubic crystalline form when it is sintered. The cooling process from cubic to tetragonal leads to an expansion of 2.3% and tetragonal to monoclinic of 4.2%. These expansions result in cracks formation, so there is a need to stabilize the tetragonal form. By adding a small amount of yttria to the zirconia, the most prevalent way of stabilizing the tetragonal phase and maintaining zirconia in a metastable condition at room temperature is achieved, which is called transformation toughening.[9]
Zirconia reinforced ceramics has an excellent aesthetic quality, biocompatibility, and mechanical property. It has mechanical properties of 1200 HV hardness, 900-1200 MPa flexural strength, and fracture toughness of 6-8 MPa. It has higher strength even when tooth preparation volume is small during making a crown. Moreover, compared to gold, zirconia is less costly. [10] However, the dental restoration’s long-term clinical success is affected by the mechanical property, aesthetic quality, and biocompatibility, and by fitting the margin. A large marginal gap leads to a crown’s failure by dissolving dental cement so quickly that plaques readily accumulate, causing marginal leakage. [11] The marginal gap usually refers to the space between the restoration margin and preparation margin. Microleakage is passing the bacteria, fluids, molecules, or ions between the tooth structure and the restorative material. [12] Factors that affect the crown’s fittings such as; fabrication design, place of the margin, quality of the milling machine, milling bur, cement space, and image capturing system that are reported through in vitro and in vivo studies. [13–20]
The marginal adaptation of dental restorations has been proven to be one of the significant factors causing secondary caries and changing the composition of subgingival microflora that contribute to periodontal disease onset. The clinically permissible marginal adaptation for the dental restoration was reported to range between 17 to 120 μm. [21, 22] Therefore, chamfer and shoulder margins were suggested to make accurate anatomic contour crowns. [23]
Destructive and non-destructive techniques can measure the marginal gap of the restorations. They can be checked clinically using a mirror, probe, and appropriate illumination and magnification. Radiograph and epoxy resin replica using light and scanning electron microscopy are considered as indirect methods. The prepared tooth can be cross-sectioned and evaluated directly to assess the cement space. Modern micro-computed tomography (micro-CT) is employed as a non-destructive method of measuring the marginal gap.
The marginal space of the crowns fabricated from various Zirconia systems differs across studies. It is necessary to review the literature on the marginal space of the zirconia crowns and compare the marginal fit among different systems. Hence this study aimed to review the published literature examining the accuracy of the marginal fit of the zirconia crown and comparing the marginal adaptation between various systems to identify which of them would achieve a better marginal fit.
Materials and Methods
Ethical Approval: The proposal of the study was submitted to Riyadh Elm University’s research center, and Institutional review board approval was obtained (FUGRP/2020/150/98/97).
Research Strategy
In the present study, the research was carried out in February 2020 in PubMed and Scopus databases. The research question is, “In abutment teeth, which zirconia system is more accurate in the marginal adaptation?” The PECO is P= abutment teeth. E= one zirconia system. C= other zirconia systems. O= accuracy in marginal adaptation. The research is limited to English-language and peer-reviewed articles published from 2010 until 2020. The following combination of keywords used: (“marginal accuracy,” “marginal fit,” “marginal gap,” “marginal discrepancy,” “fitting accuracy,” and “zirconia crown”). Titles and abstracts were examined to identify articles that fulfill the inclusion criteria designed for this review. The criteria involved studies evaluating marginal adaptation of zirconia crowns through clear experimental protocols, retrospective, and prospective studies.
Inclusion Criteria
Selection of Studies
The titles and abstracts were reviewed from the studies found in the search described above, considering the inclusion criteria. After selection, the full texts of the studies were acquired. The full-text publications were screened according to the inclusion and exclusion criteria, and 16 studies were included in the review (Figure 1, Table 1). The data collected from the studies included: Author, Year, in vivo/vitro, abutment teeth, Restoration type, Restoration material, number of specimens per group, Preparation type, Cement spacer, Impression type, Scanner, CAD software, CAM machine, Fit assessment method, number of measuring points per abutment, and Marginal gap.
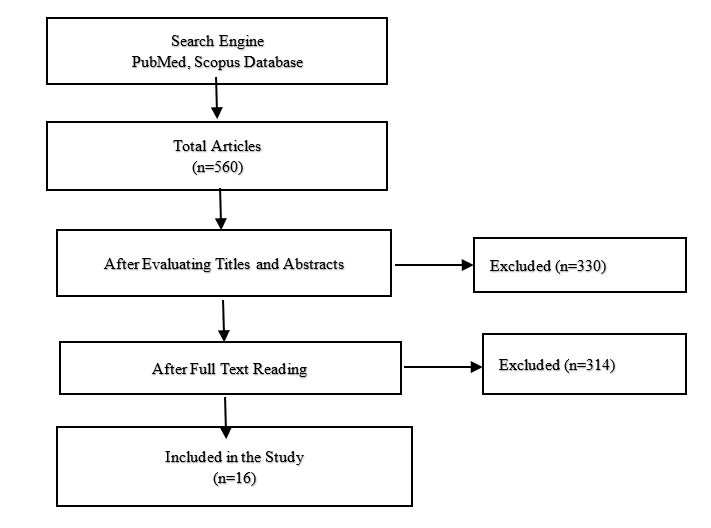
Figure 1: Search Strategy of the Systematic Review
Table 1. Overview of the Included Studies and their Setting Parameters and Results
|
Authors |
System |
Imp |
Abutment |
Evaluation |
Spacer |
N |
F. L |
Fit |
SD ± |
ACC |
|
|
Hamza et al. [24]
|
In Coris TZI |
Dig
|
PM
|
DM
|
50 μm
|
6
|
SH
|
89.30 |
2.30 |
39.30 |
|
|
Ceramill Zolid |
69.40 |
7.10 |
19.40 |
||||||||
|
Zenostar zirconia |
75.10 |
8.20 |
25.10 |
||||||||
|
Prettau zirconia Zirkonzahn |
72.80 |
8.90 |
22.80 |
||||||||
|
Bruxzir solid zirconia |
77.30 |
11.40 |
27.30 |
||||||||
|
Riccitiello et al. [25] |
Katana zirconia |
Conv |
PM |
MCT |
30 μm |
15 |
C |
66.00 |
32.33 |
36 |
|
|
Habib et al. [26]
|
Ceramill Motion 2 |
Dig
|
M
|
DM
|
20 μm
|
12
|
C
|
31.30 |
15.10 |
11.30 |
|
|
Wieland ivoclar |
42.33 |
16.90 |
22.33 |
||||||||
|
Cerec Incoris TZI |
36.55 |
17.80 |
16.55 |
||||||||
|
Zirkonzahn |
44.83 |
28.70 |
24.83 |
||||||||
|
Cad4dent |
31.36 |
19.60 |
11.36 |
||||||||
|
Hamid Jalali et al. [27]
|
Cercon |
Conv |
PM |
DM |
30 μm |
24 |
narrow SH |
71.00 |
16.00 |
41 |
|
|
round SH |
80.00 |
10.00 |
50 |
||||||||
|
Tariq F. Alghazzawi et al. [28] |
Zahnfabrik |
Conv |
M |
S |
30 μm |
30 |
SH |
36.00 |
14.00 |
6 |
|
|
Rafael Schlögel Cunali et al. [29]
|
Ceramill Motion 2 |
Dig |
M |
SR
MCT |
20 μm |
20 |
C |
77.90 68.73 77.83 74.83 |
12.21 8.86 16.13 6.84 |
57.90 48.73 57.83 54.83 |
|
|
Cerec incoris TZI |
|||||||||||
|
Rocio Ortega et al. [30]
|
Nobel Procera |
Conv
|
PM |
S
|
50 μm |
40 |
C |
41.09 |
7.45 |
41.09 |
|
|
Lava 3M Zircon |
49.48 |
10.91 |
49.48 |
||||||||
|
VITA In-Ceram |
65.63 |
34.59 |
15.63 |
||||||||
|
Sibel Cetik et al. [31] |
Ceramill Motion 2 |
Conv
Dig |
M T |
S |
45µm |
60 |
SH C
|
C-S 79.0 C-C 101.4 D-S 53.70 D-C 84.90 |
C-S 39.93 C-C 17.17 D-S 24.01 D-C 24.01 |
C-S 34 C-C 56.40 D-S 8.70 D-C 39.90 |
|
|
Balaji N Rajan et al. [32]
|
CERAMILL motion |
Dig |
M T |
S |
40 μm |
20 |
SH |
83.00 |
6.77 |
43 |
|
|
InCoris TZI |
68.00 |
1.77 |
28 |
||||||||
|
Min-Kyung Ji et al. [33]
|
- Zirkonzahn |
Dig |
PM T |
DM |
30 μm |
48 |
SH C
|
118.8 |
78.20 |
88.80 |
|
|
-ZENOSTAR®ZR |
40.50 |
41.50 |
10.50 |
||||||||
|
Syed Rashid Habib et al. [26]
|
Ceramill Motion 2 |
Dig |
M T |
S |
30 μm |
100 |
Deep C |
46.93 |
13.50 |
6.93 |
|
|
Wieland, Ivoclar |
56.38 |
30.14 |
26.38 |
||||||||
|
Cerec, inCoris TZI |
81.75 |
11.71 |
51.75 |
||||||||
|
Prettau Zirconia, Zirkonzahn |
101.7 |
35.56 |
71.65 |
||||||||
|
75.47
|
46.67
|
45.47
|
|||||||||
|
Cad4dent |
|||||||||||
|
Ediz Kale et al. [15]
|
Zenostar |
Dig |
M |
DM |
Cement space 40 μm |
48 |
SH |
41.00 |
38.00 |
1 |
|
|
CBCT |
44.00 |
42.00 |
4 |
||||||||
|
3D |
60.00 |
58.00 |
20 |
||||||||
|
Raúl Euán et al. [34] |
Lava™ 3M ESPE |
Conv |
M |
DM |
Cement space 20 μm |
20 |
SH |
59.83 |
11.28 |
39.83 |
|
|
C |
76.97 |
7.55 |
56.97 |
||||||||
|
Lorena Oliveira et al. [35]
|
Metoxit |
Dig |
M T |
SR |
10 μm |
10 |
C |
59.20 |
14.30 |
49.20 |
|
|
Conv |
71.10 |
19.10 |
61.10 |
||||||||
|
Dig on cast |
87 |
31 |
77 |
||||||||
|
Syed Rashid Habib et al. [36]
|
CERCON |
Dig |
M |
DM |
30 μm |
40 |
SH |
199.5 |
40.72 |
169.50 |
|
|
C |
214.5 |
44.85 |
184.46 |
||||||||
|
Shoko Miura et al. [37]
|
Cercon Smart Ceramics System |
Conv |
M T |
SR |
30 μm |
15 |
cervical SH |
70 |
30 |
40 |
|
|
round SH 0.2 |
80 |
30 |
50 |
||||||||
|
round SH 0.5 |
80 |
40 |
50 |
||||||||
|
Dig: Digital, Conv: Conventional, M: Molar, PM: Premolar, S: Section Technique, MCT: Micro-CT, SR: Silicon Replica Technique, DM: Digital Microscope, 3D: 3D scan technique, SH: Shoulder finish line, C: Chamfer finish line, T: Typodont, ACC=Accuracy |
|||||||||||
Table 2. Overview of the intraoral scanners (IOS), CAD software, CAM machine, and zirconia materials used in the studies.
|
CAD Software |
CAM Machine |
Zirconia Material |
|
|
Ceramill Map400 [29] Cerec inLab [29,32] Cercon Eye [36] 3Shape Trios [26,31,35] S600 ARTI (Zirkonzahn) [33] ZENO TEC® System [33] 3D laboratory scanner[15] Optical Lava™ Scan[34] Ceramill scanner [37] 3Shape D700 [35] N/S [24,38] |
Cercon Art[36] Dentsply Sirona[29] 3Shape software 27 Ceramill 33 Cerec [32] ZirkonzahnArchiv software[33] Dental Designer; Wieland[33] inCoris Zi33 Trios 3Shape22 Cercon® art[37] Optical Lava™ [34] Cares System Straumann[25] N/S[15,24,26,38] |
Cercon Brain[36] Dentsply Sirona33 3Shape software27 Ceramill (Ceramill (motion)[29,32] Cerec blanks (in coris TZI) 25,[33] Milling machine (Zirkonzahn) [32] 3shape D250[33,35] inCoris Zi33 Cercon® brain[37] Lava™ Form[34] MCXL DentsplySirona[24,38] Ceramill(Ceramill motion2) 34 Weiland34 Zirkonzhan34 S1 VHF machine34 Cares System Straumann[25] N/S11,20 |
CERAMILL Motion25 CERAMILL Motion233 Ceramill Zolid34 Wieland, Ivoclar20,22 Cerec InCoris TZISirona[24,26,29,32,38] Zenostar Ivoclar[15,24,33] Bruxzir (10AN)[24] Katana Kuraray[25] Zirkonzahn22,25,[33],33,34 Cad4dent Nacera[26,39] Lava 3M[30,34] Cercon Dentsply Sirona[27,36,37] Zahnfabrik VITA[28] Nobel Procera[30] VITA In-Ceram[30] Metoxit[35] |
|
N/S: not specified; Note: Some of the studies used the addition silicone impression material[21,23–27,30,32] |
|||
Statistical Analysis
The descriptive data are shown as numbers and frequencies. The fit was the mean of marginal gaps in the studies and accuracy was obtained by subtracting fit from the pre-set spacer. Mean values were calculated, resulting from the weighted individual group mean value and the number of test specimens per-group.
Results
The sixteen studies included in the analysis for this review presented a single crown. Four different fit measuring techniques were used: silicone replica technique (three results), sectioning technique (five results), digital microscope (seven results), and Micro-CT technique (Two results) (Table 1). The scanners, CAD software, CAM machines, and zirconia materials are described in (Table 2). Eight of the results had a conventional impression, and ten of them were based on digital techniques. The total mean value of all systems was 67 μm, and the accuracy is 36 μm, which was within the acceptable clinical range.
Discussion
The study’s purpose was to review the published literature investigating the accuracy of the marginal fit of a zirconia crown and comparing the marginal adaptation between different systems. According to McLean et al. (1971), the clinically permissible marginal fit is within 120 μm. [21] In an earlier review on the fit of CAD/CAM restorations, published in 2014, the marginal gaps ranged from 39 to 201 μm. [40] These results support the findings of the present study. Our study was mainly based on literature published between 2010 and 2020, and the marginal fit ranged from 31 to 214 μm. A previous study recommended using chamfer and shoulder margins to make the exact anatomic contour of crowns. The mean fit of chamfer and shoulder finish lines are 69 μm and 72 μm, respectively. It was concluded that the marginal fit of zirconia copings with either shoulder or chamfer finish line shows no significant differences. One of the limitations of this study was the lack of standardization to compare conventional impression techniques with the intraoral scanner. Some studies reported that the intraoral digital scanning provided a lower mean gap value than conventional impression and gypsum cast scans. It can be assumed that one of the factors that contributed to decreased marginal discrepancies in some systems is the prostheses were set to the correct position without any friction against the abutments as the correct positioning of the prosthesis requires more cement space. So, the marginal discrepancy is affected by the cement space. In our review, die spacer values ranged between 10 μm-50 μm, the mean marginal fit was 72 μm and 77μm, and the accuracy was 62 μm and 27 μm, respectively. Additional studies are necessary to investigate the optimal cement space required for lower marginal discrepancies within clinically acceptable ranges.
Processing devices are distinguishable by milling axis numbers: 3-axis devices, 4-axis devices, and 5-axis devices. It has been reported that the five-axis dry milling CAM produces better marginal accuracy but takes more time. [24] The highest marginal discrepancy was recorded in group Incoris TZI, which was milled with the MXCL milling machine with a 4-axis motion. It explains the significant difference between Incoris TZI and other systems included in the study. Another critical factor in determining the marginal adaptation is the balance between the shrinkage of pre-sintering blanks and the final sintered zirconia. According to an earlier review, a short sintering time had no effect on zirconia coping’s marginal fit. [41] Hence different porcelain-veneering techniques that might lead to changes in zirconia copings’ marginal fit were introduced within the dental ceramics. [42] A comparison accuracy of the fit of zirconia-based prostheses fabricated by two CAD/CAM systems, including layering, press-over, and CAD-on techniques, was performed. The results indicated important alterations in all three techniques; however, these alterations were in the range of clinically permissible marginal adaptation. The changes were smallest using the press-over technique and significant compared with the conventional layering technique. About marginal fit, evaluating the zirconia coping was more reliable than on veneered zirconia to determine the system fabrication precision. In the literature, it is mentioned that the cementation techniques may influence the marginal fit due to the variation in cement material viscosity as well as seating forces. Moreover, there is a considerable debate whether using a resin or conventional glass ionomer cement in zirconia crowns. The universal resin cement showed good precision performances irrespective of the restorative material.
Four different fit measuring techniques were used: silicone replica technique, sectioning technique, digital microscope, and Micro-CT technique. Incoris TZI has a marginal gap of 78, 69, 89, and 75 μm, respectively. With the limitations of other factors in this study, the least marginal gap was observed in the sectioning technique. According to the presented results, the Cercon system showed the highest marginal discrepancy (Fit 114 μm; Accuracy 84 μm), and Zahnfabrik is the least (Fit 36 μm; Accuracy 6 μm). These study findings may be related to differences in evaluation methodologies such as microscopes, microscope magnification, measurement location, number, or luting agents. However, some studies compared only marginal discrepancy values at two points of zirconia-based prostheses. It is difficult to infer that these values represent the complete accuracy for the fit of the prosthesis. More precise and meaningful conclusions will be drawn if marginal discrepancy values are compared in many points. All specimens produced in-vitro studies were examined under ideal conditions that may not simulate the oral condition.
Within the study’s limitations, it can be concluded that all the Zirconia systems considered in this study produced marginal discrepancy within the clinically desirable range. However, the Cercon system recorded the highest marginal discrepancy, and Zahnfabrik was the least. The marginal fit of zirconia copings with either shoulder or chamfer finish line did not significantly differ in marginal discrepancy. Further, reviews and meta-analyses concerning the internal adaptation, marginal gap, and the optimal cement space of crowns fabricated by various zirconia systems are recommended.
